Quick Access
Autologous reconstruction uses tissue from the patient herself to create the new breast. We can use skin, adipose tissue, and muscle from different parts of the body depending on the patient’s build. These procedures are particularly indicated when there are alterations in the thoracic skin, as in some patients undergoing radiotherapy. The reconstructed breast will increase or decrease in volume, depending on weight gain or loss.
An advantage of these procedures is that, in most cases, we avoid the use of external or artificial tissue and achieve a natural and stable result over time.
Types of autologous reconstruction
RECONSTRUCTION WITH PATIENT’S OWN FAT (LIPOFILLING)
Autologous breast reconstruction using a patient’s own fat is called “lipofilling”. We use the patient’s own fat obtained by liposuction from other parts of the body (saddlebags, abdomen, and thighs) to improve and reshape the breast. Once the fat has been obtained, we subject it to a component separation process to then inject micro-grafts of fat into the breast to correct the areas that we have selected.
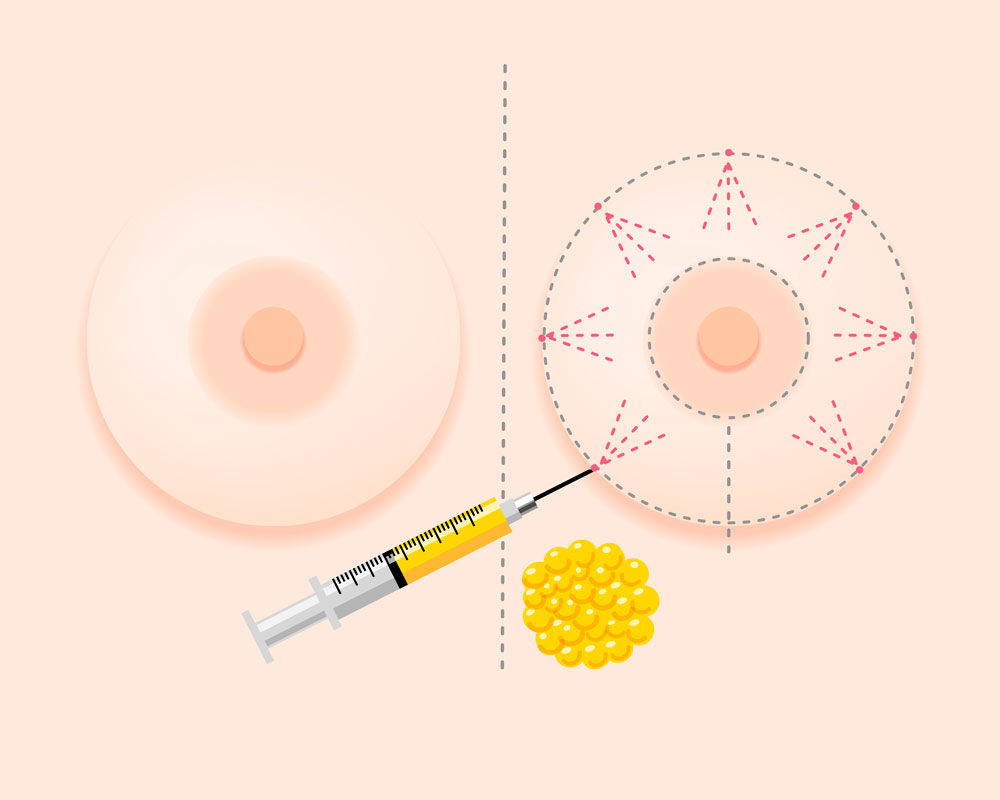
This technique allows treating small areas of retraction and subsidence that may appear after conservative treatment, and it can serve as a complement to breast reconstruction with implants or as an exclusive technique for breast reconstruction, associated with other autologous procedures.
RECONSTRUCTION WITH LARGE DORSAL (LATISSIMUS DORSI)
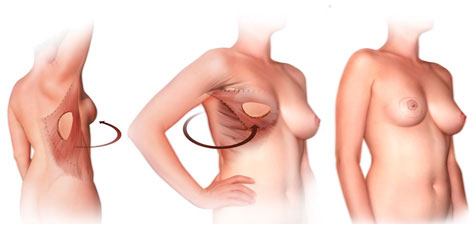
In this type of reconstruction, a section of skin and fat is obtained attached to the large dorsal muscle of the back and rotated to the chest, maintaining its original vascularity.
This type of reconstruction may require the simultaneous use of a breast prosthesis or its own fat if sufficient tissue supply is not achieved to form the new breast. The scar on your back will be located at a height where it is easily covered by your bra or swimsuit. The procedure is performed under general anesthesia with a duration between 2 and 3 hours, and the hospital stay lasts 3 to 5 days.
MICRO-SURGICAL RECONSTRUCTION: DIEP
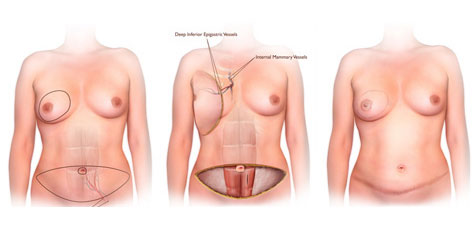
The reconstruction is performed exclusively with skin and abdominal fat without altering the musculature. Dissection of the deep inferior epigastric artery perforator flap(DIEP) is performed. Once the free flap is obtained, it is placed in the chest, and the vessels (artery and vein) are joined to the internal mammary vessels of the chest through microsurgery. Subsequently, the tissue is remodeled to acquire the consistency and shape of a new natural-looking breast.
For planning this technique, the Breast Pathology Center has the most advanced imaging technology. Magnetic resonance imaging and vascular CT allow the study the vascularization of the tissues to be transferred, notably increasing the speed and safety of the procedure in the operating room.
The procedure lasts between 6 and 8 hours and requires an admission of 7 to 10 days.